In 10 seconds? Comparing young people with high and lower risk of bipolar disorder (BD), researchers observed how their thinking processes and parts of their brains started to differ over time. This could help predict who will experience the disorder.
Why is this significant? The study's goal was to be able to predict who will experience a manic episode ("the high" in bipolar disorder) just by looking at changes in people's brains and behavior. The paper suggests that brain networks affecting mood and cognition are strengthening over time in young people who have no close relatives with BD. However, among those, who have a close family member (parent or sibling) with bipolar disorder, these networks were weaker, even without experiencing a manic episode. For those, who have had mania the differences were even more prominent.
OK, so regretfully, some people are more susceptible. What can we do with this? It is important to discover more about the onset of bipolar disorder – because our knowledge about it is still patchy. This research reinforces the view that we need to screen high-risk people and help them avoid serious illness. Scientist will now also explore how the knowledge of physical changes in the brain can help design therapies and find out who is more resilient to the illness. (Having a close family member with BD means one’s risk is about 10 times higher than for other people). Although some patients have learned to manage bipolar, episodes can be detrimental to the general health, finances, and social connections of patients and their families. People can be out of work for weeks or months as a minimum but in extreme cases, episodes can lead to suicide. The findings also remind us that more research is needed into the underlying mechanisms of bipolar disorder.
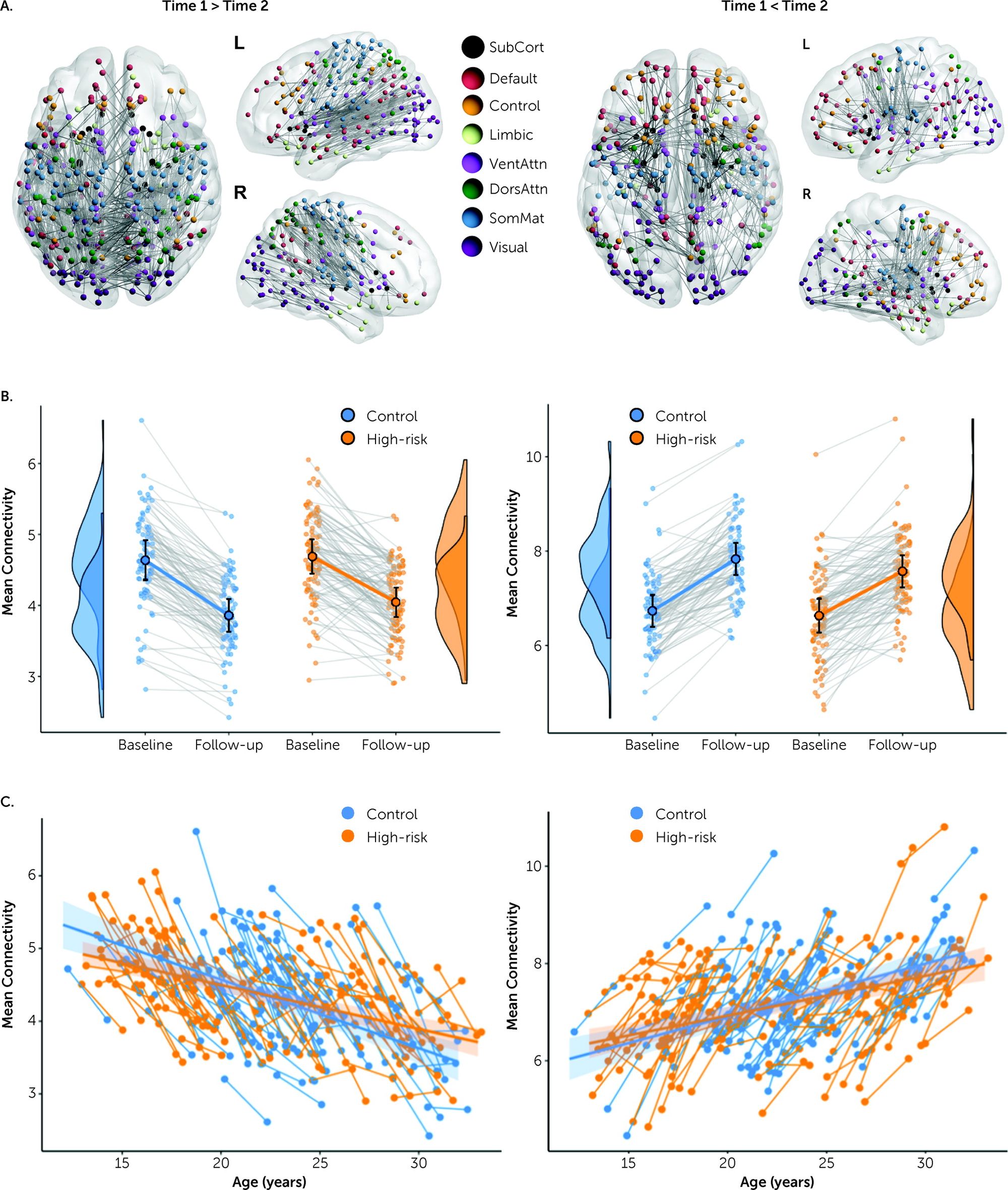
OK, and how did they make this discovery? The team has recruited people 183 'affected' young people in 12-30 years age range ('affected' means people with a first-degree relative with BD) and 97 'unaffected' individuals (no family history of mental illness). The reserchers picked this age group because this is the time in our lives when our brains mature and the time of the first onset of episodes. They performed an MRI brain scan and repeated it after 2 years to observe the changes in structural connectivity (grey matter linking different regions of the brain) and followed up the groups for 10 years. This is how they've found that as the young people aged, the connectivity in the high-risk group members' brains weakened, whereas it got stronger in the control group. A few participants experienced manic episodes and their relevant brain connections became even weaker.
Hang on, bipolar physically changes the brain? Yes. A study from 2021. has found structural changes in the brains of people who have already had several manic episodes. The researchers have even pinpointed the area, the frontal cortex, AKA the frontal part of the outer layer of the brain, responsible for emotion regulation and executive control. This area became thinner for people who have experienced several episodes of mania. Another finding was that people with BD showed faster enlargement of brain ventricles – cavities that contain cerebrospinal fluid, the leakage of which can lead to headaches or meningitis. This research was also a longitudinal study, tracking participants between six months and nine years with two MRI scans performed on their brains. Earlier studies have also found structural brain changes, for example, a decreased amygdala in young BD patients. (The amygdala is an almond-shaped part of the brain that is primarily linked to emotional processes.)
I’ve got a close relative with bipolar and I’m starting to get concerned… OK, I did not want to alarm you! Consider this: while estimates say that 4.4 percent of the US adult population experiences bipolar disorder over their lifetime, having a first-degree relative does not mean that you will actually develop it. Studies say only a small portion of people with first-degree relatives (4.5-22.4%) will experience the illness. In addition, most patients don't have a positive family history because there are several non-genetic factors: changes in sleep and circadian rhythms, stressful events, substance abuse, and even some character traits. Other factors can be mood swings, anxiety disorders, and the presence of attention deficit hyperactivity disorder (ADHD).
Is there a way to prevent bipolar episodes?
According to our current scientific knowledge, bipolar episodes (mania or depression) cannot be prevented. This is a lifelong condition. However, both doctors and patients can take steps to avoid symptoms escalating into severe psychosis.
It helps to identify early warning signs and triggers and seek medical help. (For example: losing appetite, social withdrawal, frequent headaches or on the contrary, feeling hungry, irritable, having more energy than normal, and problems with sleep). Sticking to prescribed mood-stabilizing medications, regular checkups, and behavioral counseling can all lower the impact and shorten episodes.
Coping strategies can help patients control symptoms and their lives. Find some tips about a ‘wellness toolbox’ here or contact these organizations in the US: NAMI HelpLine and DBSA Chapters/Support Groups for support.
Endre Szvetnik has distilled 7 research papers, saving you 24.5 hours of reading time
The Science Integrity Check of this 3-min Science Digest was performed by Dr. Ángel V. Jiménez.






