In 10 seconds? Researchers have found that stem cells originating in bone marrow can play a key role in successful pregnancies. They hope that the discovery can become a basis for a new fertility treatment.
What exactly did they discover? The study confirmed that it’s not just egg-producing ovaries and a uterus hosting the embryo that is needed for a successful pregnancy. Following the successful fertilization of an egg, stem cells arriving from the bone marrow to the uterus transform its lining and help the implantation of the embryo. How? They become decidual cells (essential for getting and staying pregnant). If this transformation does not occur, the pregnancy will terminate.
What mechanism is at play here? It’s so-called mesenchymal stem cells that perform this vital function. Interesting fact: they've been known as stem cells that can grow into bones, cartilage, and fat. It turns out they also help transform the endometrium, the inner lining of the uterus. A damaged endometrium can result in repeated lost pregnancies or infertility and the findings raise the hope of science being able to fix this condition.
So, how did they discover this? Working with lab mice, a research team from Yale University used a mild form of chemotherapy to wipe out the animals’ bone marrow. Earlier attempts also destroyed the mice's eggs, but the researchers have managed to refine their technique to keep them intact this time. The next step was to make two groups of mice pregnant, one before and one after a healthy bone marrow transplant to test if bone marrow played a role in pregnancy.
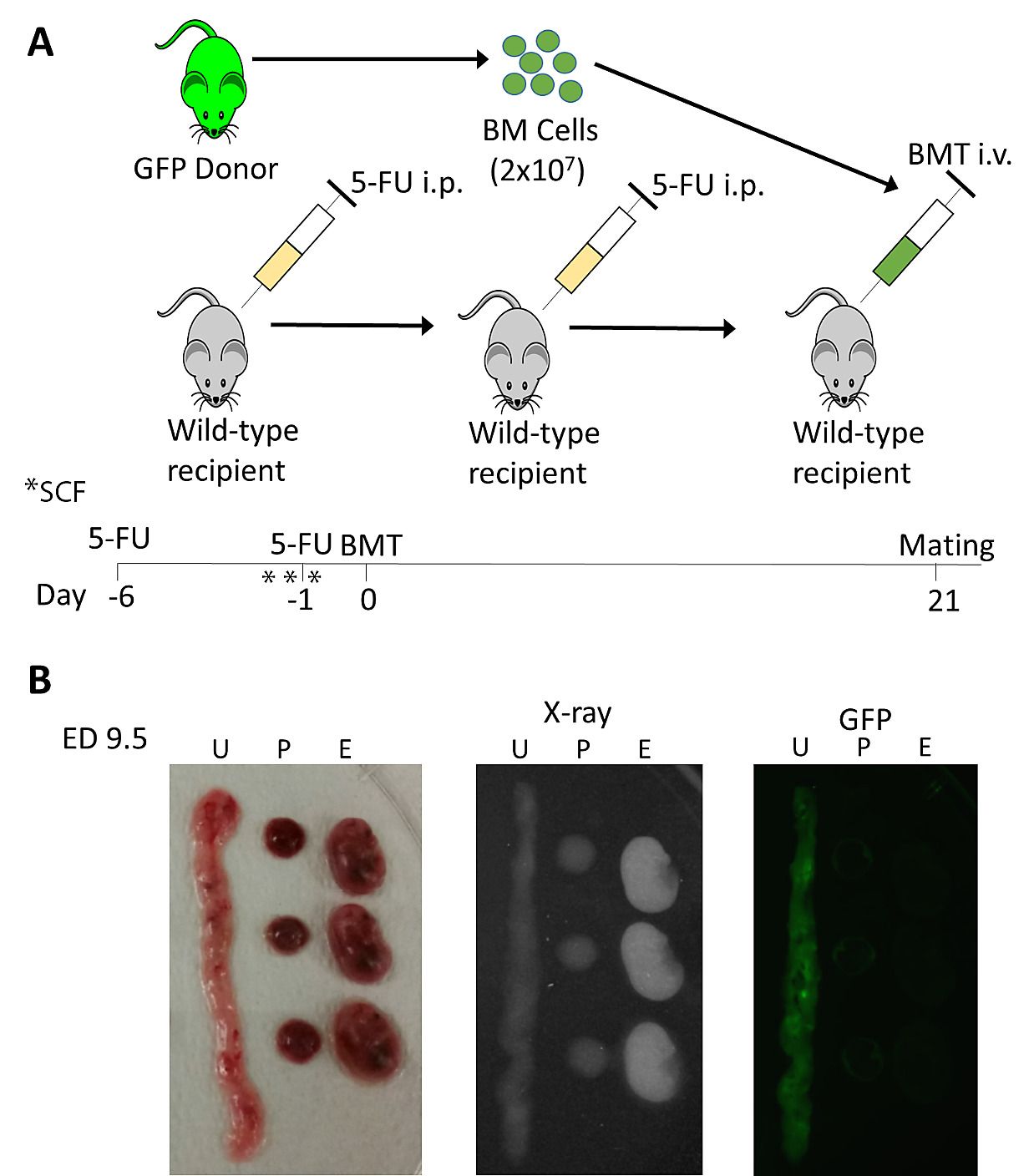
Which they proved right? Anything else they discovered? Yes! For this study, they investigated the role of the gene Hoxa11, present in both the bone marrow and the uterus and believed to help prepare the endometrium for implantation. When Hoxa11 is partially absent, lab mice cannot maintain their pregnancies and when it is completely lacking, pregnancy doesn't even start. But when partially or completely Hoxa11-deprived mice receive bone marrow transplants from healthy peers, both groups gain the ability to become pregnant.
What can we expect in the future? First a caveat: as mentioned above, the study was done in mice and was published back in 2019. Hoxa11 is worthy of further investigation before human trials can begin (by the time of writing, in 2022 none have been announced). The findings - that a bone marrow transplant from a healthy donor could improve fertility - are great news. Up to now, there’s been limited success in treating the majority of women with recurrent implantation failure and loss of pregnancies due to endometrial defects. A 2021 study reported that a technique, granulocyte colony-stimulating factor (G-CSF) combined with transcutaneous electrical acupoint stimulation (TEAS) to transfer frozen-thawed embryos has increased the thickness of the endometrium and the number of ongoing pregnancies but the method is still awaiting confirmation by randomized clinical trials. The role of bone marrow-derived stem cells was therefore welcome news – if clinical trials confirm its safety and effectiveness in humans.
Bone marrow’s other fertility card
Another surprising use of bone marrow linked to human reproduction was discovered when in 2006 a team used bone marrow-derived stem cells to create artificial early-stage sperm.
Four years later a Japanese team repeated the feat and managed to generate sperm that produced healthy and fertile mice.
For this they used a combination of proteins to convert the mice’s embryonic stem cells into so-called primordial germ cells, that would either develop into eggs or sperm.
Researchers described the studies as the first steps to producing sperm for infertile men or potentially allowing same-sex female couples to produce artificial sperm and have their own biological daughters.
Endre has distilled 6 research papers, saving you 21 hours of reading time with an evidence score of 3 out of 5*
*this is the updated version of an earlier Sparrow digest